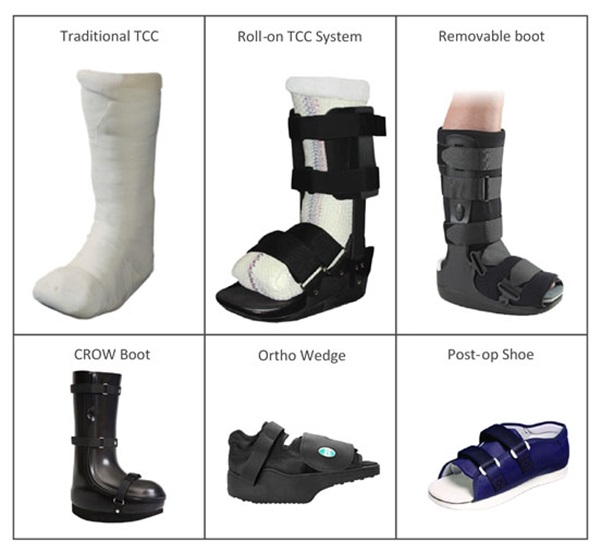
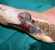
Diabetic Feet
Foot care amongst diabetics is incredibly important as foot related complications are common for those with diabetes.
Foot ulcers for example, which affect as many as 1 out of 10 people with diabetes, can all to easily develop from blisters and small wounds to posing a threat of amputation. Even small ulcers on the foot can represent a serious risk: they may heal extremely slowly and need rigorous treatment to cure. Ulcers can develop into serious lower body infections, with the possibility of amputation at an advanced stage.
Diabetic foot complications include:

Peripheral neuropathy is a condition that effects diabetics and can cause tingling, burning or numbness in your feet. This disease causes weakness, numbness and pain (usually in your hands or feet), as well as a loss of sensation that may be compared to the feeling of wearing a thick stocking.
It can be more noticeable during exercise or at night when you try to fall asleep and the tingling keeps you awake. This tingling can range from a mild curiosity to irritation to outright discomfort.
Although it may not seem too alarming, this condition can cause ulcers, infections … even amputations.

It is relatively common for people with diabetes to not feel foot problems until they have developed, therefore it is key to ensure you have regular foot examinations.
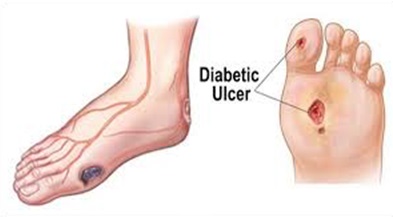
Diabetic foot ulcers represent a major complication of diabetes mellitus. They result from a raised level of blood sugar that occurs in consequence of a long-term lack of insulin. In the long term a raised blood sugar content however results in damage of foot nerves and blood vessels. In turn damaged foot nerves retard the perception of painful stimulus on the feet; minor injuries are often recognized too late.
Lesions become infected, heal badly or do not heal at all due to the disturbed blood circulation. In the worst case tissue dies and the affected limb needs to be amputated.
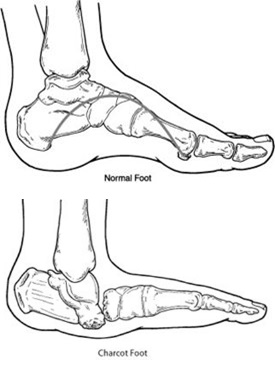
What Is Charcot Foot?
Charcot foot is a condition causing weakening of the bones in the foot that can occur in people who have significant nerve damage (neuropathy). The bones are weakened enough to fracture, and with continued walking, the foot eventually changes shape. As the disorder progresses, the joints collapse and the foot takes on an abnormal shape, such as a rocker-bottom appearance. Charcot foot is a serious condition that can lead to severe deformity, disability and even amputation. Because of its seriousness, it is important that patients living with diabetes—a disease often associated with neuropathy—take preventive measures and seek immediate care if signs or symptoms appear.
Causes
Charcot foot develops as a result of neuropathy, which decreases sensation and the ability to feel temperature, pain or trauma. Because of diminished sensation, the patient may continue to walk—making the injury worse. People with neuropathy (especially those who have had it for a long time) are at risk for developing Charcot foot. In addition, neuropathic patients with a tight Achilles tendon have been shown to have a tendency to develop Charcot foot.
Symptoms
The symptoms of Charcot foot may include:
- Warmth to the touch (the affected foot feels warmer than the other)
- Redness in the foot
- Swelling in the area
- Pain or soreness
Diagnosis
Early diagnosis of Charcot foot is extremely important for successful treatment. To arrive at a diagnosis, the surgeon will examine the foot and ankle and ask about events that may have occurred prior to the symptoms. X-rays and other imaging studies and tests may be ordered. Once treatment begins, x-rays are taken periodically to aid in evaluating the status of the condition.
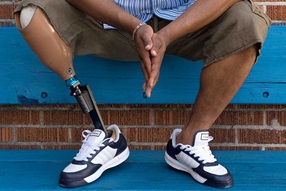
When Is Amputation Necessary?
Even with preventive care and prompt treatment of infection and complications, there are instances when amputation is necessary to remove infected tissue, save a limb or even save a life.
Taking care of your feet
We know that people with diabetes have a much greater risk of developing problems with their feet, due to the damage raised blood sugars can cause to sensation and circulation. So we encourage you to keep an eye on your feet at home and make sure that you get a quality foot check from a properly trained person at least once a year. This is the code for the specific 70% 30% layout.
Top tips for healthy feet
- Have a quality foot check by an appropriately trained person at least once a year. You should always take your shoes and socks off so that they can do a proper assessment.
- Don’t be self-conscious about your feet.
- After the foot check, ask what your risk is of developing foot problems.
- If you are at increased risk of foot problems, make sure you have been referred to a foot protection service or specialist podiatrist for expert input.
- Check your feet every day - look for any signs of redness, pain, build-up of hard skin or changes in the shape of your feet. Find out more about how to spot foot problems.
- Be aware of any loss of feeling in your feet because you may not feel if you hurt your feet.
- Ask someone at home to monitor the feeling in your feet by doing the quick, easy Touch the toes test. This can be done between appointments and if there are any changes go to your GP. The Touch the Toes test is not a substitute for the annual foot review.
- Look after your toenails.
- Do not use corn-removing plasters or blades as these can damage healthy skin.
- Use moisturising cream every day and wear well-fitting shoes that protect and support your feet.
- Always examine the inside of your shoes for sharp objects or stones before putting them on and replace ruffled innersole linings. Avoid socks, stockings or tights with wrinkles or prominent seams.
- Garters and stockings or socks with elastic tops should also be avoided because they may restrict the circulation. Never wear socks with darned areas or holes.
- Know who to call at the first sign of any new foot problem.
Steps you can take to prevent problems happening
- If you smoke, get support to help you stop because smoking affects blood circulation and so increases your risk of developing serious foot problems.
- Keep good control of your blood glucose, blood pressure and cholesterol levels.
- Eat a healthy diet that is low in saturated fat, sugar and salt, and high in fruit and vegetables.
- Make sure you attend your annual foot check.
- Know your risk of developing foot problems and if you have been referred to a foot specialist for expert advice.
- Attend all your appointments.
- Follow our top tips for healthy feet.
- Make sure that your socks and shoes are comfortable and fit well.
- If you are able to, take regular physical activity, for example a brisk walk each day.
- Contact your GP or diabetes team if you have any concerns about your feet - don’t wait until your annual foot review.
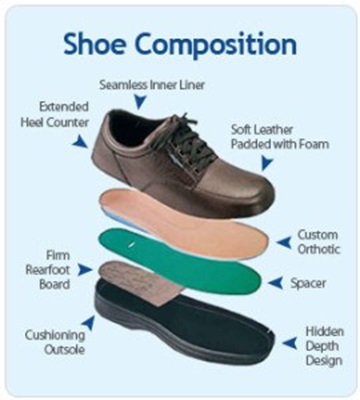
If you are in the early stages of diabetes, and have no history of foot problems or any loss of sensation, a properly fitting shoe made of soft materials, with a shock absorbing sole, may be all that you need. It is also important for patients to learn how to select the right type of shoe in the right size, so that future problems can be prevented.
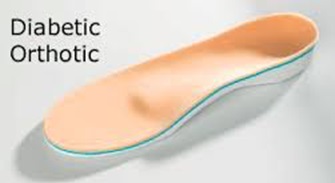
Once a person with diabetes develops an ulcer, they are at risk for an ulcer in that location for the rest of their life. This is due to the fact that when skin heals, it will never return to its original strength. Since we have learned this, podiatrists work to take special precautions with these areas of the foot.
One way that we do this is through orthosis. Many times when people hear about orthotics they think about inserts that change the position of the foot, diabetic orthosis are a little bit different.
They are molded to fit the shape of your foot exactly so that there is no space between your foot and the surface of the orthosis. This serves to prevent any areas of increased pressure. Now, if you have an area that has had an ulcer in the past or is more prone to one, then your podiatrist will take the proper steps to provide extra accommodations for that area.
(TCC) is a specially designed cast designed to take weight off of the foot (off-loading) in patients with diabetic foot ulcers (DFUs). Reducing pressure on the wound by taking weight of the foot has proven to be very effective in DFU treatment